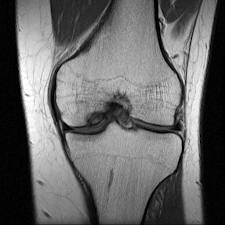
Knee Avascular Necrosis (AVN)
Tampa, Saint Petersburg, Clearwater, FL & Beverly Hills, Los Angeles, California
Avascular necrosis (AVN) also referred to as osteonecrosis of the knee can be a debilitating progressive disease of the knee in which the subchondral bone loses vascular supply and a portion of the bone dies.
This can lead to subchondral collapse resulting in severely erosive degenerative arthritis. Initially, it was felt to be a disorder that involved predominantly the medial femoral condyle of the knee. Now, researchers have expanded the concept to include three distinct pathological entities:
- Spontaneous AVN or osteonecrosis.
- Secondary AVN or osteonecrosis.
- Post arthroscopic AVN or osteonecrosis.
Idiopathic or Spontaneous osteonecrosis has an unknown etiology. However, there are many theories including interruption of the arterial supply, capillary occlusion, interosseous capillary tamponade, or injury to a vessel wall.
There is some controversy that It occurs more frequently after age 50, and is much more common in females. Nearly three times more females than males are afflicted.
Spontaneous AVN is mostly seen in the epiphyseal region. In the knee this is generally seen in the medial or lateral tibial plateau, or in the medial or lateral femoral condyle. Spontaneous AVN also has been seen following a du corgi la insufficiency fracture.
Secondary avascular necrosis may involve both femoral condyles with multiple lesions in the epiphysis, metaphysis, and diaphysis of the bone. Usually, this occurs in the younger subset less than 45 years of age and may be bilateral in greater than 80% of the time. Risk factors for secondary avascular necrosis include radiation, chemotherapy, and also trauma. Medical disorders such as myeloproliferative diseases, sickle cell disease, are associated with increased risk of AVN.
Indirectly, there is a correlation between corticosteroid use; however, close examination of the data on corticosteroid use is conflicting and it may be similar to alcohol use in that it is inconsistent and that sometimes very little quantities are associated with this. Not all patients who have large doses of corticosteroids develop this similarly to the risk factor for alcohol use, as avascular necrosis only occurs in 10% of patients on high dose corticosteroids and in a much lower percentage in the general population that abuses alcohol.
Post arthroscopic avascular necrosis is believed to result from the laser heating up the bone and then resulting in osteonecrosis. It has also been postulated that trauma during the actual surgery can precipitate it as generalized trauma is an associated risk factor. Post arthroscopic avascular necrosis has a similar lesion to spontaneous osteonecrosis and is found in the epiphysis as opposed to secondary osteonecrosis with multiple lesions at multiple sites including the epiphysis, metaphysis and diaphysis of the bone. In post arthroscopic avascular necrosis, there is no predominant age group and it has been seen with a variety of arthroscopic procedures. Early in the stages of this condition, radiographs do not reveal the lesions in 20% of the cases and once the condition is visible on radiographs or x-rays, it has already progressed to a later stage and the knee may have already collapsed.
Magnetic resonance imaging (MRI) is a much more sensitive diagnostic tool for detecting lesions and assessing the bone marrow viability as well as the distribution of the lesions. It is suggested that patients with knee AVN who have associated minor pain in the hip should undergo an MRI of the hip to evaluate if there is a concomitant hip avascular necrosis or osteonecrosis developing. This also should be done in patients with hip avascular necrosis who start complaining of knee pain. Evaluation of the knee should then be undertaken.
Dr. Lox has seen cases of avascular necrosis of the knee or osteonecrosis from a variety of disorders and comments that most patients who have already had surgical procedures generally wish to avoid joint collapse if at all possible and avoid total knee replacement.
Alternative therapies such as regenerative medicine with PRP and stem cell therapy are of great interest to patients who wish to prevent total knee replacement and provide an alternative treatment strategy. Dr. Lox suggests that each patient should have a comprehensive evaluation and rehabilitation program to address their individual needs as regenerative procedures such as platelet-rich plasma and stem cell therapy should be tailored appropriately for each patient’s individual need based upon their situation.
If avascular necrosis is caught early and has not progressed to joint collapse, obviously this is a better prognosis than if the joint has subsequently collapsed and treatment options are less favorable.
Dennis M. Lox, M.D., serves patients in the greater Tampa Bay area, including, Clearwater, St. Petersburg, Tampa, New Port Richey, Sarasota, Orlando and Spring Hill.
He also has an office where he performs stem cell therapy in the Los Angeles Metropolitan area of Beverly Hills, California to accommodate the needs of patients on an international level.
Located in the 33765 area, our offices can be reached at (727) 462-5582 (Clearwater). Call for immediate assistance or schedule your visit online today.